Mariana Rico-Restrepo, Medical Director, Americas Health Foundation
Why We Developed the Latin America Vaccination Scorecard
Few public health interventions have transformed human health as profoundly as vaccination. Over the past five decades, vaccines have saved an estimated 154 million lives worldwide and continue to prevent millions of deaths every year. These numbers represent children who grew up healthy, families that remained whole, and communities able to prosper because diseases were prevented.
Yet vaccination programs often become victims of their own success. Because many societies today have not witnessed the devastating consequences of diseases such as measles, polio, or diphtheria, the perceived risk of these illnesses has diminished. When the threat becomes less visible, public attention to immunization weakens, and maintaining strong vaccination systems requires constant vigilance.
In Latin America, this dynamic is particularly relevant. The region has historically maintained a strong culture of vaccination through robust National Immunization Programs (NIPs), regional cooperation, and support from institutions such as the Pan American Health Organization (PAHO). These efforts have contributed to historic public health achievements, including the elimination of poliomyelitis and the interruption of endemic measles transmission.
However, recent years have shown the fragility of these advances. Outbreaks of previously controlled diseases have reemerged in several countries, coverage gaps persist across the region, and inequities in access are significant. Additionally, broader global trends, including shifts in funding priorities and evolving public narratives around vaccines, are creating new pressures on NIPs.
These realities motivated the Americas Health Foundation (AHF) to develop the Latin America Vaccination Scorecard, with the support of Pfizer. The initiative was designed to assess how vaccination systems are functioning across the region and to identify concrete opportunities for strengthening them. Our intention was not merely to produce another report or diagnostic exercise. Rather, we wanted to generate a clear and comparable picture of the status of vaccination programs and, more importantly, to help translate these insights into action.
By examining the institutional foundations of NIPs across eight Latin American countries, the Scorecard aims to provide policymakers, public health leaders, and civil society organizations with practical insights into where systems are performing well, where gaps remain, and what steps could strengthen protection for populations across the region. Ultimately, our objective is that these findings and recommendations will help reinforce political commitment to immunization and accelerate the transition toward stronger, more resilient vaccination systems across the life course. The full regional report, detailed country profiles, and accompanying infographics can be downloaded at: https://www.americashealthfoundation.org/projects/cmbfoxtqd001az9u6906n3jy5
How the Vaccination Scorecard Works
Vaccination coverage is often discussed in terms of individual vaccines or national coverage rates. While these metrics are essential, they do not fully capture the broader institutional and policy environment that determines whether immunization programs succeed.
NIPs depend on a wide range of components: legal frameworks, financing mechanisms, surveillance systems, data infrastructure, communication strategies, and service delivery models. When one of these elements is weak, it can undermine the effectiveness of the entire system.
The Latin America Vaccination Scorecard was designed to evaluate these structural dimensions. Rather than focusing exclusively on coverage, the Scorecard examines the policy and system architecture that supports vaccination across the region.
The project assessed NIP frameworks in eight Latin American countries: Argentina, Brazil, Chile, Colombia, Ecuador, Guatemala, Mexico, and Peru.
Seventeen indicators were developed to capture key dimensions of vaccination systems. Each indicator was scored using a standardized rubric from 1 to 5 and weighted according to its relative importance. The results were then aggregated to produce a composite score for each country, allowing for comparison across the region.
Indicators examined multiple aspects of immunization programs, including the existence of national vaccination policies and legal frameworks, the functioning of national immunization technical advisory groups (NITAGs), the availability of digital vaccination registries, financing mechanisms, adverse event surveillance systems, public communication strategies, and the transparency and accessibility of vaccination data.
Data were compiled exclusively from publicly available official sources from the past decade, including national Ministry of Health documents, immunization schedules, WHO and PAHO databases, and published research.
To complement this desk research, AHF convened multidisciplinary expert roundtables in each country. These discussions brought together policymakers, clinicians, public health specialists, and representatives of civil society to validate the findings, clarify contextual issues, and provide additional insight into implementation challenges. By combining quantitative scoring with expert dialogue, the project sought to create a robust and realistic picture of vaccination systems across Latin America.
Key Regional Findings
The results of the Scorecard highlight both important achievements and significant gaps.
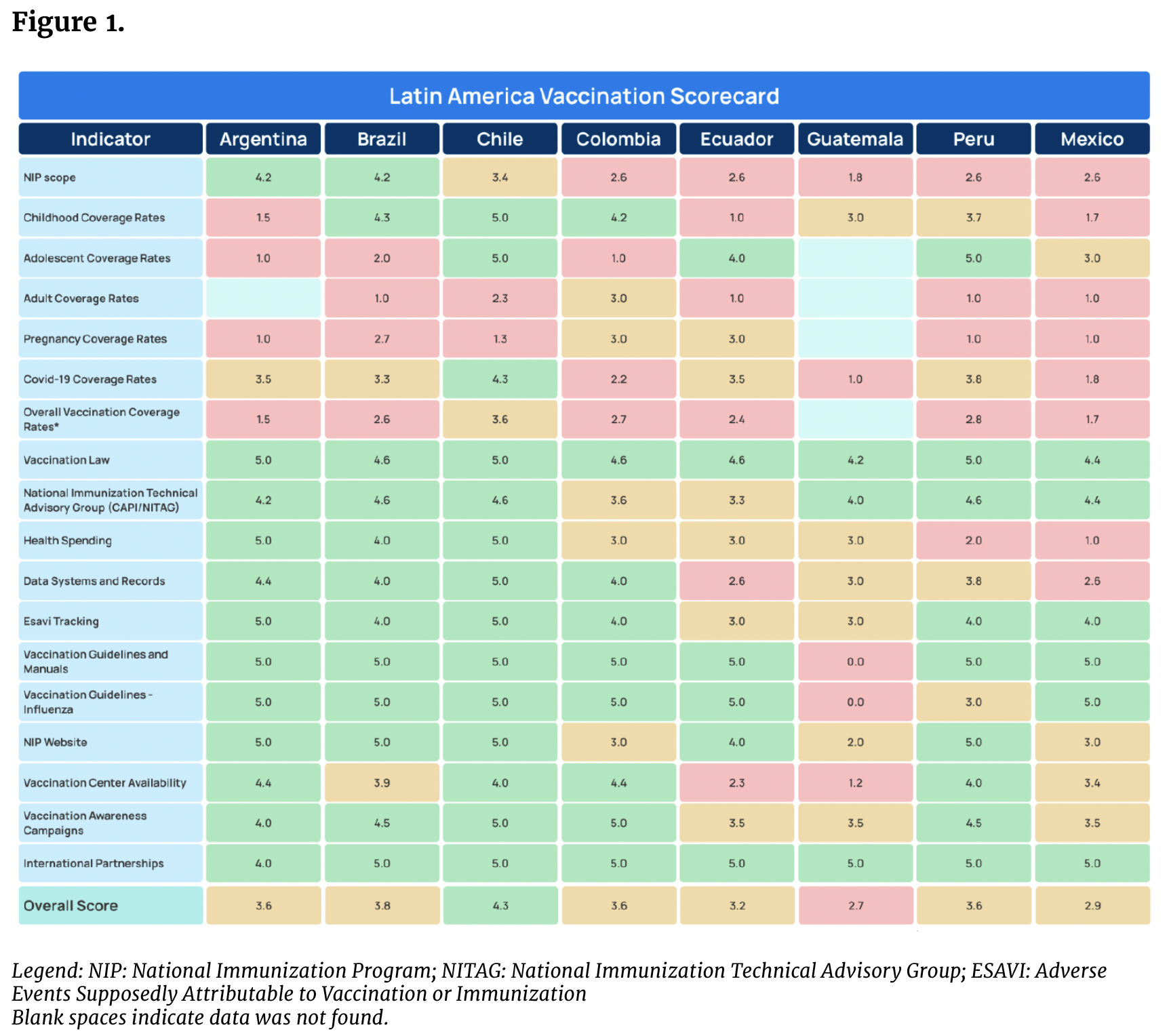
Across the eight countries analyzed, composite scores ranged from 2.7 to 4.3 out of 5, with a regional average of 3.5. These results reflect a broader regional pattern: many countries have strong institutional foundations for NIPs, but implementation issues limit their effectiveness.
Figure 1 illustrates the regional Scorecard results, providing a visual comparison of how the eight countries scored across the indicators.
Governance
The Scorecard findings highlight that most countries in Latin America have established the core governance structures necessary to support strong NIPs, including national vaccination policies, legal frameworks, and technical advisory bodies. However, the effectiveness of these governance arrangements varies considerably across countries. In most cases, gaps exist in policy coordination, institutional leadership, and the regular review and updating of national immunization strategies.
NITAGs play a particularly important role within this governance architecture by providing independent scientific guidance on vaccine policy, including recommendations on vaccine introduction and updates to immunization schedules. While all of the countries analyzed have established NITAGs, the Scorecard findings suggest that their institutional strength and influence vary considerably. In several cases, limited resources, irregular meeting schedules, or weak integration into national decision-making processes reduce their ability to fully inform vaccination policy.
Strengthening the governance of NIPs will require reinforcing the technical and institutional capacity of NITAGs, ensuring that their recommendations are systematically considered in policy decisions, and establishing regular processes for reviewing and updating NIP calendars. Strong governance structures are essential for enabling evidence-based decision making, coordinating stakeholders across the health system, and ensuring that immunization policies remain responsive to evolving public health needs.
Life-Course Vaccination
One of the most consistent findings across countries was the continued strength of pediatric vaccination programs. Early childhood vaccination remains the backbone of NIP efforts in Latin America, and most countries continue to maintain relatively robust schedules for infants and young children.
In contrast, vaccination strategies for adolescents, adults, older adults, and pregnant women remain significantly less developed. Many NIPs still operate primarily under a pediatric model of immunization, with limited institutional adaptation to life course vaccination approaches.
Even in countries with relatively high overall scores, important gaps persist in adult and maternal vaccination coverage, as well as in the availability of reliable data for these populations.
This imbalance reflects both historical and structural factors. NIPs in Latin America were originally designed with a strong focus on childhood vaccination, and much of the institutional architecture, including funding mechanisms and performance indicators, remains oriented toward pediatric coverage.
Financing
Financing for NIPs is often insufficient or fragmented. Vaccine procurement budgets are often not adjusted as the programs expand their scope; and in many countries, resources for implementation such as workforce training, outreach, communication campaigns, and surveillance are limited. Additionally, resources specifically allocated for life-course strategies are not in place in most countries.
Data Systems
Data systems and epidemiological surveillance are incomplete, particularly beyond early childhood vaccination. While most countries maintain relatively robust monitoring systems or registries for pediatric vaccines, the availability of reliable coverage data for adults, older adults, and pregnant women remains limited. In many countries, national reporting systems do not systematically track vaccination coverage for these populations, and epidemiological surveillance for vaccine preventable diseases is still largely oriented toward childhood indicators.
This gap has important implications for public health planning. Without consistent and disaggregated data, it becomes difficult for health authorities to accurately assess population immunity, identify coverage gaps, or design targeted vaccination strategies for vulnerable groups. The absence of reliable surveillance and monitoring systems for maternal and adult vaccination also limits the ability of governments to evaluate program performance, forecast vaccine needs, and allocate resources efficiently.
Although several countries have begun implementing digital vaccination registries, these systems are not always fully operational or interoperable across health institutions. Reporting delays, incomplete data entry, and fragmentation between public and private providers further limit the ability of policymakers to track vaccination coverage accurately or respond quickly to emerging gaps.
Access and Education
The Scorecard revealed persistent inequities in access, particularly among rural populations, migrants, and marginalized communities. Structural barriers such as geographic distance, limited availability of vaccination sites, and restricted service hours limit access for many populations. In several countries, vaccination services are primarily offered during standard working hours, which can make it difficult for working adults and caregivers to attend appointments. Addressing these inequities will require more flexible service delivery models, including extended clinic hours, expanded vaccination sites, and targeted outreach strategies that reduce the social, economic, and geographic barriers that continue to affect immunization uptake across the region.
In terms of communication, many countries rely heavily on campaign-based messaging during outbreaks or vaccination drives, but sustained education efforts to reinforce the value of routine immunization are less common. As a result, vaccination communication is often reactive rather than proactive, focusing on short term responses to emerging threats instead of building long-term public understanding and confidence in immunization. Strengthening communication strategies will require continuous engagement with communities, clear public health messaging about the benefits of vaccines across the life course, and better integration of communication efforts into routine healthcare delivery.
The Importance of a Life Course Approach
Perhaps the most important insight from the Scorecard is the need to transition toward a life course approach to immunization. As populations in Latin America age and the epidemiological profile of the region evolves, vaccination strategies must expand beyond childhood. Protecting adults, pregnant women, and older adults will become increasingly important for preventing disease, reducing health system costs, and protecting vulnerable populations.
The life course approach recognizes that vaccination is not a one-time intervention in early childhood but a continuous strategy for maintaining health throughout life. Achieving this shift will require adjustments in policy, financing, service delivery, and public communication. Health systems must integrate vaccination systematically into primary care services, prenatal care programs, and adult health initiatives and ensure healthcare personnel are up to date on vaccination recommendations for all age groups.
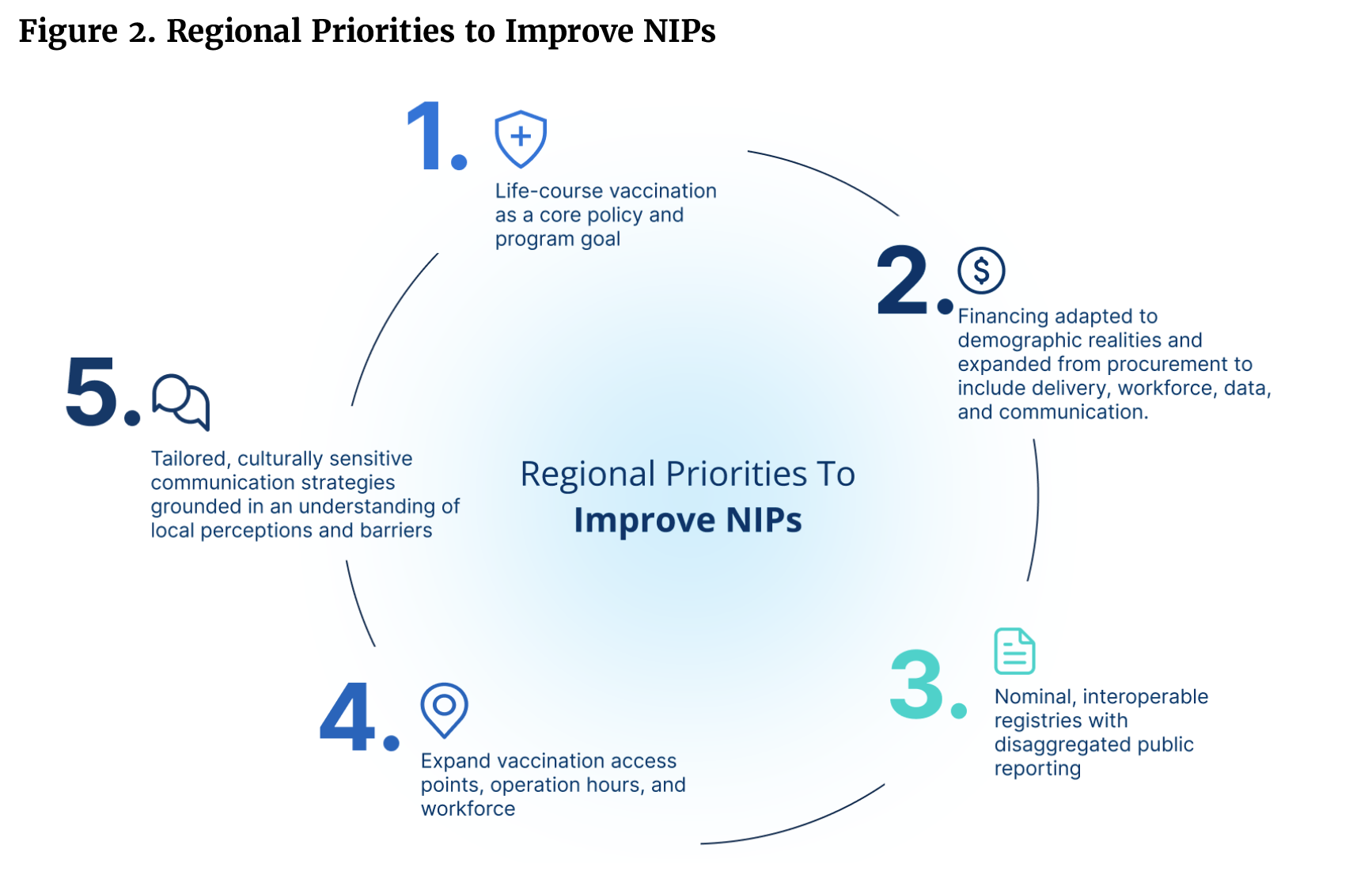
Figure 2 outlines the key regional priorities identified through the Scorecard for strengthening NIPs.
Why This Project Matters
The Latin America Vaccination Scorecard is not intended to rank countries or assign blame. Rather, its goal is to support evidence-based policy dialogue and encourage collaboration across the region.
By identifying where systems are strong and where they require reinforcement, the Scorecard provides a practical tool for policymakers and public health leaders seeking to strengthen immunization programs.
Equally important, the project demonstrates the value of regional cooperation. Many of the challenges identified in the Scorecard are shared across countries. Addressing them will require collective solutions, including the exchange of best practices, coordinated research, and sustained political commitment to vaccination.
At AHF, we believe that strengthening vaccination systems is one of the most important investments countries can make in the health of their populations. Immunization protects individuals, reduces the burden on health systems, and contributes to broader social and economic development.
Looking Forward
The findings of the Vaccination Scorecard highlight both the resilience and the vulnerability of immunization programs in Latin America. The region has strong foundations: experienced public health institutions, decades of successful vaccination campaigns, and a deep culture of regional collaboration. These strengths must be reinforced through continued investment, improved data systems, and policies that expand immunization across the life course. Protecting the progress achieved over the past decades will require renewed commitment from governments, healthcare professionals, researchers, and the general public.